JOINT FORCES
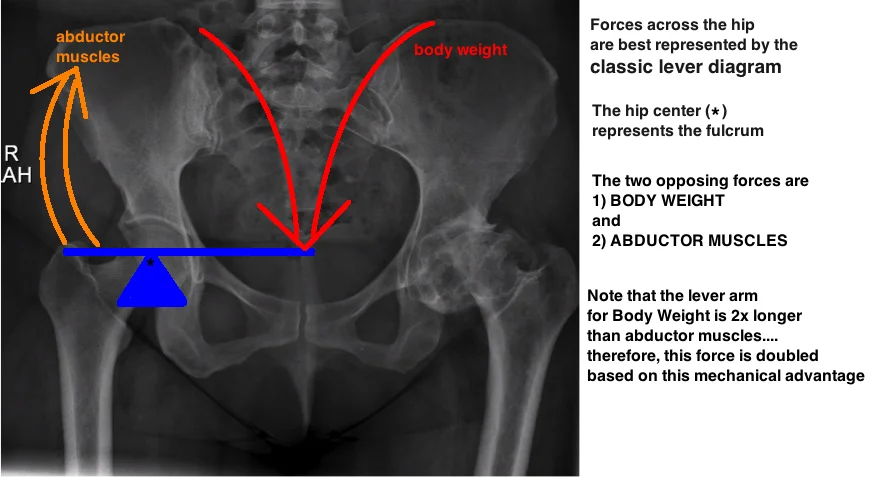
The normal hip joint is best understood as a Lever-Arm (see picture).
The hip center is the fulcrum that sits between 2 opposing forces:
Lever arm #1 is the distance from the hip center to the center of body weight.
Lever arm #2 is the abductor mechanism, which is distance from the hip center to the greater trochanter (aka the insertion point of our abductors).
These two lever arms oppose each other. In a normal hip, the body weight lever arm is 2.5 times longer than the abductor, which means that the abductor force must be 2.5 times stronger than body weight. The greater the body weight, the more force across the hip joint by multiple factors. This is one theoretic correlation between obesity and hip arthritis.
Joint reactive forces depend on the activity. Force of walking is 2.5x body weight, force of jogging is 6x body weight, force of running is 8x body weight.
clinical: In progressive hip degeneration, the head begins to collapse, the neck shortens, and the abductor mechanism loses tension causing weakness and pain due to increased joint reactive forces. In designing the first modern hip reconstruction, Dr. Charnley wanted to change the forces across the hip center by deepening the acetabulum (shortens Lever arm #1) and performing a troch-slide osteotomy (lengthen Lever arm #2). But there is no free lunch in medicine and deepening the acetabulum increases bone loss, osteotomizing the greater troch slows rehabilitation and requires greater soft tissue dissection. Current techniques for hip reconstruction focus on restoring the anatomical geometry of the hip—placing the acetabular component in a low and medial position to restore the center of rotation and selecting a femoral stem that will restore offset (maximizing tension of the abductors) and leg length.
PELVIC TILT
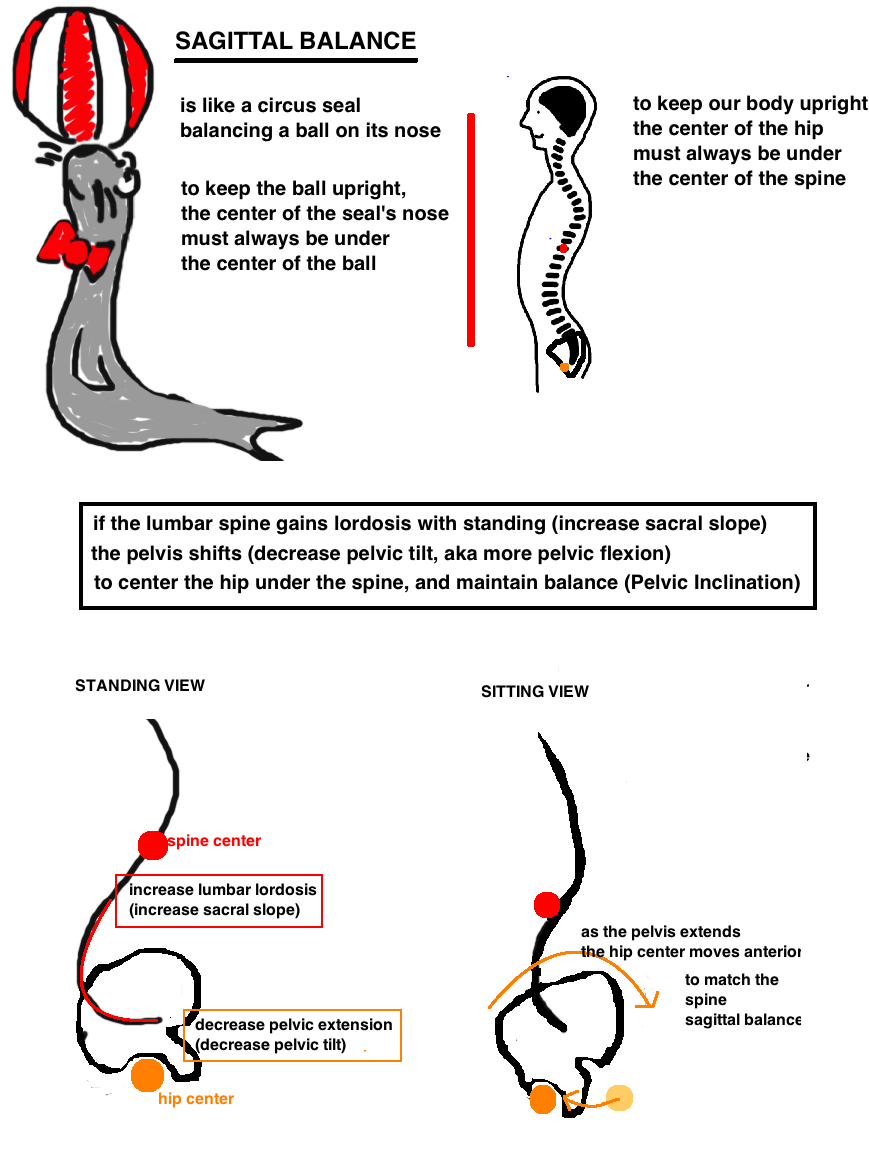
Acetabular orientation is not fixed. There is a dynamic relationship between the pelvis and the lumbosacral spine, which moves in a predictable way, from standing to sitting, to maintain sagittal balance.
The basic concept is that pelvic tilt and sacral slope are dynamic pelvic parameters (change with body position), but their sum represents the Pelvic Incidence, which is static (always the same number regardless of position).
The Pelvic Incidence is a fixed number in adults, it represents overall body balance. Yet as we move into different positions (sitting, standing, lying down), the SS and PT change in order to maintain PI.
When standing, the amount of lumbar lordosis increases (SS increases), so the pelvis tilts forward, ie flexes (represented as a decreasing PT).
During sitting, the Pelvis Tilts backwards (ie extends) causing increased PT. Increasing Pelvic Tilt Increases Acetabular Anteversion (at a rate of 1.0° pelvic tilt to 0.7° of anteversion) [6]. Increasing the anteversion prevents anterior impingement (its important to avoid anterior impingement bc it causes the femoral head to lever out posteriorly). During sitting the lumbar lordosis decreases (SS decreases).
The SS and PT change by the same amount in a normal flexible spine-sacrum to maintain the PI (balance). Sitting after THA risks posterior dislocation because of anterior impingement, therefore, a mobile lumbo-pelvic segment is essential to minimizing THA dislocation. However, Lumbar Fusion reduces lumbo-pelvic motion and risks THA dislocation. The more lumbar segments fused, the less lumbo-pelvic flexibility and the higher the dislocation risk: No fusion: 1.5% risk. 1-2 levels: 2.7% risk. 3-7 levels: 4.6% risk [7, 8].
Lets look more at the measurements to describe the orientation of pelvis [9].
Pelvic incidence (PI) is the main axis of sagittal balance of the spine (ranges 48° - 53° ). It is the angle between Line 1 (perpendicular to Sacral Prominotry, aka superior plate of S1) and Line 2 (center of Sacral prominitory to Hip Center)
Sacral slope (SS) is the angle of the sacrum. Angle between Line 1 (line parallel to sacral prominotry) and Line 2 (a horizontal reference line)
Pelvic Tilt (PT) is the angle of the pelvis. Angle btwn Line 1 (center of Sacral prominitory to Hip center) and Line 2 (a vertical reference line). As the upper pelvis moves posterior, the pelvic tilt increases, therefore pelvic tilt can be thought of as the degree of pelvic extension. When the upper pelvis tilts forward (anterior flexion), there is less pelvic tilt. Pelvic tilt does not change after THA. With normal saggital balance (PI), the PT should be < 22°.
REFERENCES
1. Lewinnek, G.E., et al., Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg Am, 1978. 60(2): p. 217-20.
2. Biedermann, R., et al., Reducing the risk of dislocation after total hip arthroplasty: the effect of orientation of the acetabular component. J Bone Joint Surg Br, 2005. 87(6): p. 762-9.
3. Dorr, L.D., et al., Combined anteversion technique for total hip arthroplasty. Clin Orthop Relat Res, 2009. 467(1): p. 119-27.
4. Kosashvili, Y., et al., Acetabular alignment and primary arc of motion for minus, skirtless, and skirted 28-, 32-, 36-, and 40-mm femoral heads. J Arthroplasty, 2013. 28(2): p. 279-285 e2.
5. D'Lima, D.D., et al., The effect of the orientation of the acetabular and femoral components on the range of motion of the hip at different head-neck ratios. J Bone Joint Surg Am, 2000. 82(3): p. 315-21.
6. Lembeck, B., et al., Pelvic tilt makes acetabular cup navigation inaccurate. Acta Orthop, 2005. 76(4): p. 517-23.
7. Perfetti, D.C., et al., Prosthetic Dislocation and Revision After Primary Total Hip Arthroplasty in Lumbar Fusion Patients: A Propensity Score Matched-Pair Analysis. J Arthroplasty, 2016.
8. DelSole, E.M., et al., Total Hip Arthroplasty in the Spinal Deformity Population: Does Degree of Sagittal Deformity Affect Rates of Safe Zone Placement, Instability, or Revision? J Arthroplasty, 2016.
9. Phan, D., S.S. Bederman, and R. Schwarzkopf, The influence of sagittal spinal deformity on anteversion of the acetabular component in total hip arthroplasty. Bone Joint J, 2015. 97-B(8): p. 1017-23.